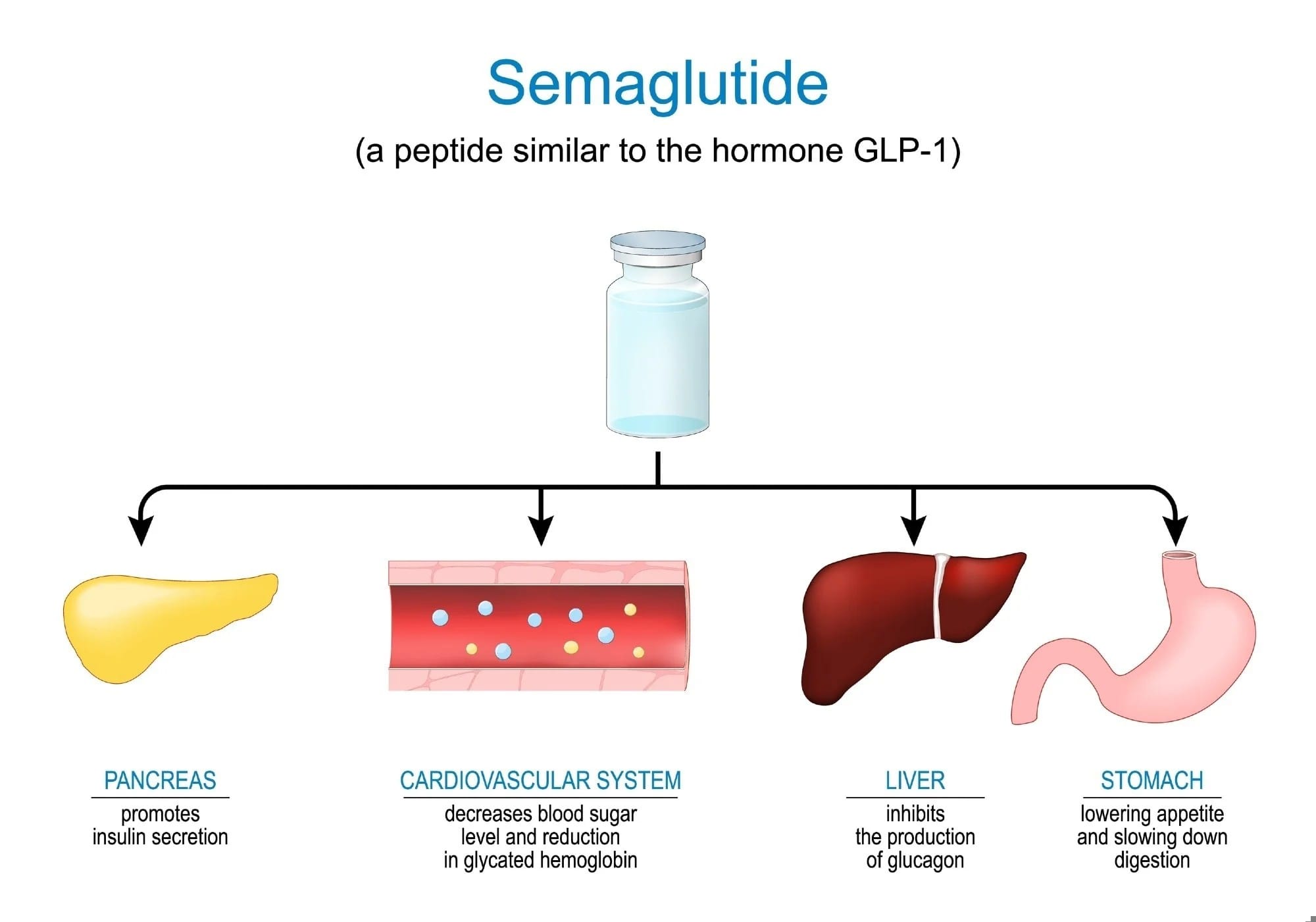
Nearly half of the United States population is affected by obesity, which is significantly associated with morbidity and mortality. With recent advancements in clinical research, anti-obesity medications such as semaglutide have demonstrated a substantial reduction in weight and other comorbid clinical factors. The authors reviewed literature and found that there is a paucity of information about healthcare expenditures with long-term use of semaglutide in clinical settings with diverse populations. Hence, this research aimed to assess how clinical outcomes and healthcare expenditures change among patients prescribed semaglutide in clinical settings.
This study extracted data from the electronic health records (EHR) of Sentara Healthcare (which included 12 hospitals across Virginia) and Yale New Haven Health System (which included 5 hospitals across Connecticut, Rhode Island). Adults of 18 years or over who were prescribed semaglutide between 1st January 2018 and 1st May 2025 were included.
The primary outcome was percentage change in body weight from baseline, which is defined as the mean values recorded during the 12 months preceding the index date. The Index date is the date when the patient received the first recorded semaglutide prescription. At least one recording of weight measurements was included at the following intervals:
Secondary outcomes measured changes in:
Additionally, medication classification (oral or injectable semaglutide) was included along with the age, gender, and race of the cohort, as it may be associated with medication and study outcomes.
A total of 23,522 patients with a mean age of 56.2 (±12.9) years were included. 66.7% were females, with 13.4% Hispanic or Latino, 1.6% non-Hispanic or Asian, 22.6% non-Hispanic Black, 59.5% non-Hispanic White, and 2.9% of other unknown ethnic background were included.
16,813 patients were from the Yale New Haven Health System (EHR obtained from 1st January 2018 to 1st May 2025), and 6709 patients were from Sentara Healthcare (EHR obtained from 1st January 2018 to 1st January 2025)
68.6% patients were diabetic, and the body mass index was calculated as weight in kilograms divided by the square of the height in meters.
Association of semaglutide prescription and cardiovascular risk factors:
(All values showed 95% of CI during result analysis)
Similar outcome patterns were seen at 24 months post-prescription period.
Healthcare expenditures were found to increase overall by $80 a month in the final 12 months of using semaglutide.
By diagnostic category, there was a $15 increase for the diseases of the circulatory system and $21 increase for the diseases of the endocrine, nutritional, and metabolic system.


Most Accurate Healthcare AI designed for everything from admin workflows to clinical decision support.