Psychotic disorders are among the most serious mental health conditions, often leading to lifelong disability, social disruption, and increased risk of premature death. For decades, research from high-income countries suggested that the incidence of schizophrenia and related psychotic disorders was stable or even declining. However, new population-based evidence from Canada challenges this assumption and points to an important shift in risk across generations.
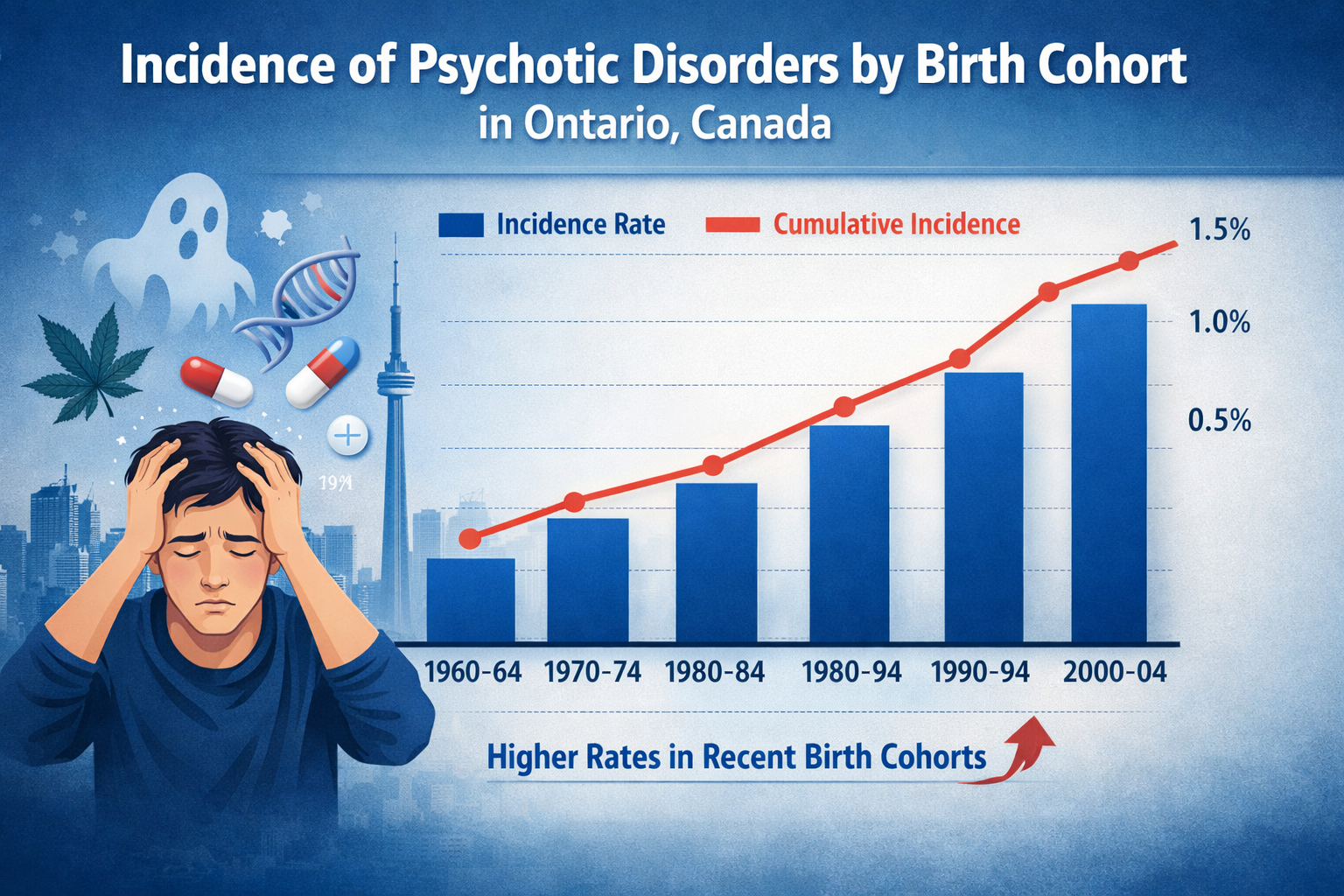
A major cohort study published in the Canadian Medical Association Journal in February 2026 examined the incidence of psychotic disorders by birth cohort in Ontario, Canada. Using health administrative data from more than 12 million individuals born between 1960 and 2009, the researchers found a clear increase in psychotic disorder diagnoses among more recent birth cohorts, particularly during adolescence and early adulthood.
This article explains the study’s findings, why birth cohort analysis matters, and what the results may mean for mental health services, prevention, and future research.
Psychotic disorders are characterized by disruptions in thinking, perception, and behavior. Common symptoms include hallucinations, delusions, disorganized thought, negative symptoms such as emotional withdrawal, and cognitive impairment. Schizophrenia and schizoaffective disorder fall under the category of schizophrenia spectrum disorders, while psychosis not otherwise specified is used when symptoms do not fully meet diagnostic criteria or when information is incomplete.
Globally, schizophrenia affects about 0.45 percent of adults, while approximately 1 percent of people in Canada live with the condition. Psychotic disorders are associated with high levels of disability, medical comorbidity, and reduced life expectancy. While genetic vulnerability plays a major role, environmental, social, and developmental factors are increasingly recognized as contributors to risk.
Most studies report trends in psychotic disorders using age-standardized incidence rates over time. While useful, this approach can obscure differences between generations. People born in different decades are exposed to distinct social, environmental, and developmental conditions that may influence mental health risk.
Birth cohort analysis examines whether individuals born in certain periods experience higher or lower risk than those born earlier, after accounting for age and calendar period. This approach helps distinguish true changes in disease incidence from changes caused by diagnostic practices, health system access, or population aging.
The Ontario study applied age-period-cohort modeling to assess whether psychotic disorder risk has shifted across generations.
The researchers conducted a retrospective population-based cohort study using linked health administrative data held at ICES in Ontario. The study included all individuals born between 1960 and 2009 who were eligible for Ontario’s public health insurance and were between 14 and 50 years of age at some point between 1992 and 2023.
Psychotic disorders were identified using hospital records and outpatient physician billing data. Diagnoses included schizophrenia spectrum disorders and psychosis not otherwise specified. To reduce misclassification of existing cases, new diagnoses required no psychosis-related care in the previous five years.
More than 12.2 million people were included, making this one of the largest studies of psychotic disorders conducted to date.
One of the most striking findings was a sharp increase in psychotic disorder incidence among adolescents and young adults. Between 1997 and 2023, the annual incidence among individuals aged 14 to 20 years increased by approximately 60 percent. In contrast, incidence rates among adults aged 21 to 50 years were stable or declined over the same period.
This pattern suggests that rising overall incidence is driven primarily by earlier onset rather than increased diagnosis later in life.
After adjusting for age and calendar period, the age-period-cohort models showed a clear and consistent increase in psychotic disorder incidence across successive birth cohorts starting with those born in the early 1980s.
Compared with individuals born between 1975 and 1979, those born between 2000 and 2004 had a 70 percent higher incidence of schizophrenia. The increase was even larger for psychosis not otherwise specified, with incidence nearly three times higher in the youngest cohorts.
These findings indicate that people born more recently are experiencing a higher underlying risk of psychotic disorders, not merely earlier detection.
The study also found that the cumulative proportion of individuals diagnosed with psychotic disorders by certain ages has increased in more recent cohorts.
By age 20, the proportion of people diagnosed with a psychotic disorder among those born between 2000 and 2004 was more than double that of those born between 1975 and 1979. By age 30, individuals born between 1990 and 1994 had a substantially higher prevalence than earlier cohorts.
At the same time, the average age at diagnosis declined by more than two years across cohorts that could be fully followed from adolescence. This shift reflects both increased incidence at younger ages and changes in how quickly individuals come into contact with mental health services.
Although psychotic disorders remain more common among males than females, the relative increase in incidence across birth cohorts was similar for both sexes. This suggests that cohort-related risk factors are broadly affecting the population rather than being limited to one gender.
The authors caution that no single factor can fully explain the observed increases. Instead, the findings likely reflect a combination of improved detection and genuine changes in risk exposure.
Ontario has significantly expanded early psychosis intervention programs since the early 2000s. These programs aim to identify and treat psychosis as early as possible, particularly among youth and young adults. Earlier detection could partly explain the declining age at diagnosis and increased use of psychosis not otherwise specified diagnoses.
However, improved access alone cannot fully account for the rising cumulative incidence and persistent cohort effects after adjusting for calendar period.
Rates of cannabis use, stimulant use, and exposure to high-potency substances have increased over time in Canada. Numerous studies link substance use, particularly cannabis, to an elevated risk of psychosis, especially among adolescents and genetically vulnerable individuals. Psychosis not otherwise specified diagnoses may capture some substance-related cases, contributing to the larger increases seen in that category.
More recent birth cohorts have experienced significant shifts in early-life environments, including urbanization, housing instability, economic stress, and exposure to adverse childhood experiences. Some of these factors are known or suspected to increase psychosis risk.
Changes in parental age, maternal health, and perinatal outcomes may also play a role. Advances in neonatal care have improved survival among infants with neurodevelopmental vulnerabilities, which could influence long-term mental health outcomes.
If the observed trends reflect a true increase in psychotic disorder incidence, the implications for health systems are substantial. Psychotic disorders require long-term, resource-intensive care, including specialized mental health services, housing support, and social assistance.
The findings support the need for continued investment in early psychosis intervention programs, youth mental health services, and prevention strategies. They also highlight the importance of monitoring emerging cohorts as they age to determine whether elevated risk persists into later adulthood.
As with all age-period-cohort analyses, disentangling the effects of age, calendar time, and birth cohort is methodologically challenging. Some earlier cohorts may have had undetected cases before the start of data availability, leading to underestimation of their cumulative incidence.
Administrative health data rely on diagnostic coding, which is not perfectly specific. However, the authors note that validated algorithms and sensitivity analyses yielded consistent results across outpatient and hospital settings.
This large population-based study provides compelling evidence that the incidence and cumulative burden of psychotic disorders have increased in more recent birth cohorts in Ontario, Canada. The rise is most pronounced among adolescents and young adults and is accompanied by earlier diagnosis.
While improved detection and access to care likely contribute, the findings raise important questions about changing social, environmental, and developmental risk factors affecting newer generations. Understanding these drivers is essential for prevention, policy planning, and ensuring that mental health systems are prepared to meet future needs.
Myran DT, Gibb M, Pugliese M, et al. Incidence of psychotic disorders by birth cohort: a population-based cohort study in Ontario, Canada. Canadian Medical Association Journal. 2026;198(4):E118–E127.
This blog article is based on an open access research article published in the Canadian Medical Association Journal. The content is summarized and interpreted for educational and informational purposes only. The original authors and publisher retain all rights to the original work. Readers are encouraged to consult the original publication for full methodological details and context.


Most Accurate Healthcare AI designed for everything from admin workflows to clinical decision support.