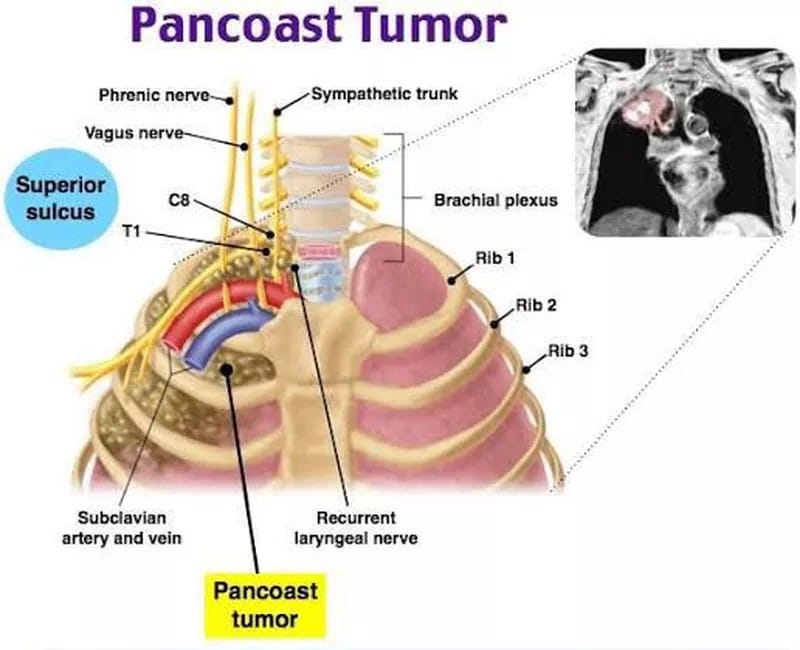
Pancoast tumors (PT) are defined as tumors that invade any of the structures at the apex of the chest, including the first rib or periosteum, the lower nerve roots of the brachial plexus, the sympathetic chain near the apex of the chest, or the subclavian vessels. Pancoast tumors occur in the apical portion of the lung, representing 3%–5% of all lung cancers.
Pancoast tumor is also known as a superior sulcus tumor. Histopathologically, these tumors are commonly adenocarcinomas, and less frequently, squamous call cancer. [1]
What causes PT?
Causes and risk factors of PT are similar to other lung cancer tumors. Common risk factors include smoking or exposure to second-hand smoke, long-term exposure to certain substances, including asbestos, radon gas, and heavy metals.
What are the symptoms of PT?
PT symptoms appear on the affected side of your body. Symptoms also depend on the structures involved in the upper thoracic region. [2]
Up to 50% of people who have PT may also develop Horner`s syndrome, which may cause:
How is PT diagnosed?
Physical examination of the upper thoracic region and its contents is vital, which includes but is not limited to the following:
Neurologic examination of both upper extremities
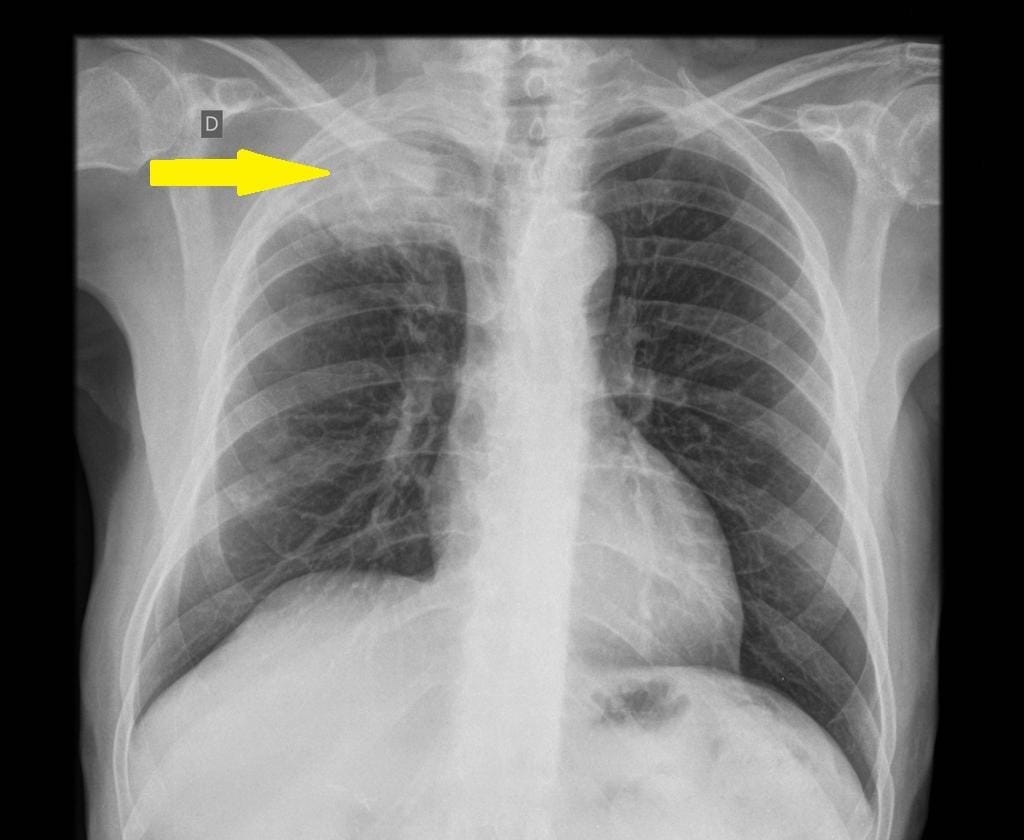
Pancoast tumor constitutes a group of malignancies (as it is classified based on location), hence a series of tests may help diagnose its status:
How is PT treated?
The Standard of care is currently chemoradiation therapy to shrink the size of the tumor, followed by surgical resection. Induction chemotherapy includes combination chemotherapeutic drugs like cisplatin/etoposide or cisplatin/mitomycin, or cisplatin/vindesine.
Contraindications to surgery include:
Extensive invasion of the brachial plexus, especially above the T1 nerve root.
In some cases, surgeons may use a combination of surgery and chemoimmunotherapy (a combination of chemotherapy and immunotherapy).
When surgery isn`t an option, your oncologist may recommend having a combination of chemoradiation and immunotherapy or stand-alone radiation therapy to slow cancer growth. [2]


Most Accurate Healthcare AI designed for everything from admin workflows to clinical decision support.