Tonsillectomy with or without adenoidectomy is one of the most common surgical procedures performed in children worldwide. Over the past two decades, surgical techniques have evolved with the aim of reducing postoperative pain, bleeding, and recovery time. One such technique is powered intracapsular tonsillectomy and adenoidectomy, commonly referred to as PITA.
While PITA has gained popularity due to its favorable recovery profile, emerging evidence suggests it may be associated with higher rates of postoperative fever. A recent prospective cohort study published in Clinical Otolaryngology sheds new light on this issue and offers important insights for clinicians and parents alike.
This article reviews the findings of that study, explains what postoperative fever means in practical terms, compares intracapsular and traditional tonsillectomy techniques, and discusses how families can be better prepared after surgery.
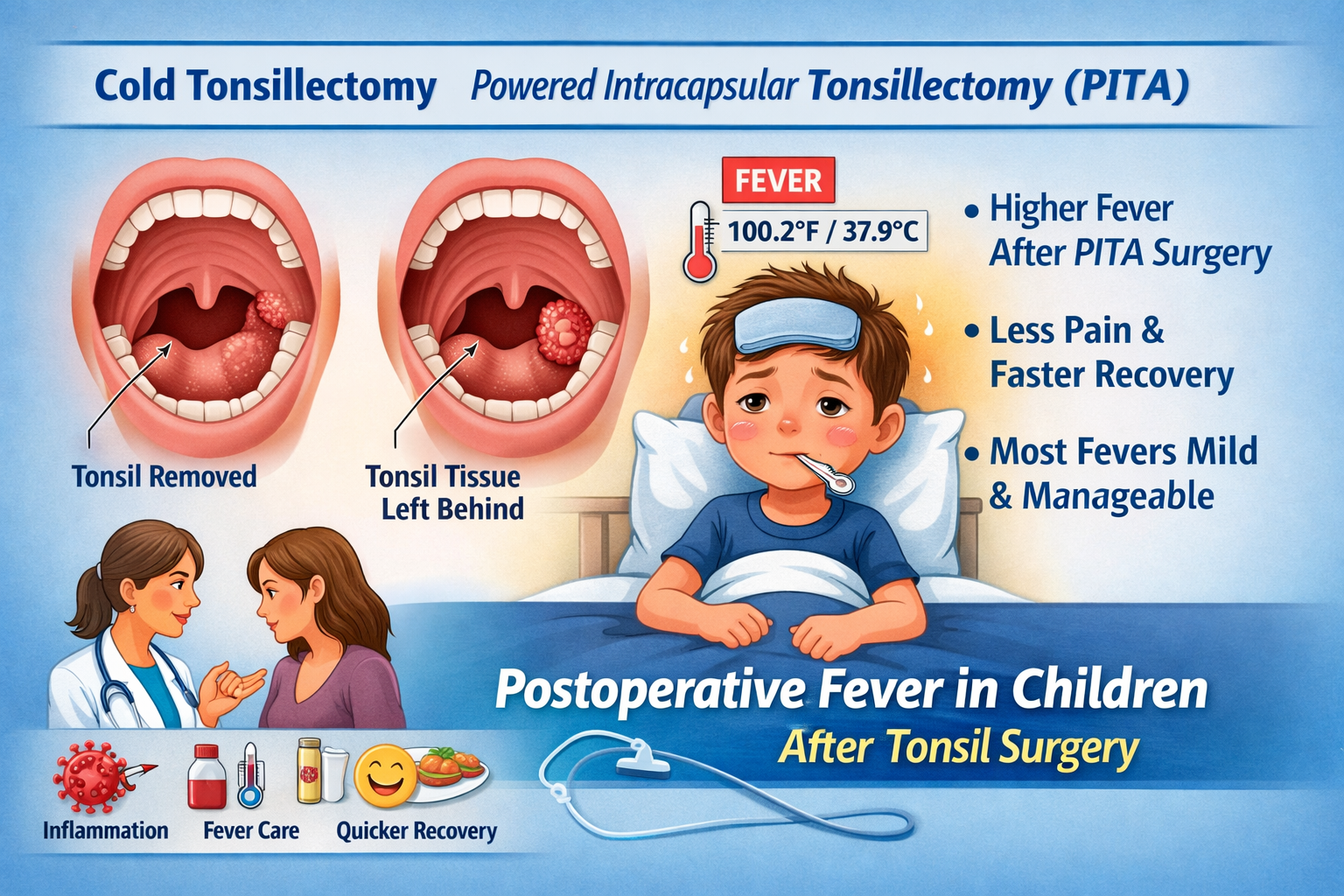
Cold adenotonsillectomy is the traditional surgical approach. The tonsils are removed completely using cold steel instruments, such as scissors or a scalpel, often followed by cauterization for bleeding control. This method removes both the tonsillar tissue and its capsule, leaving the pharyngeal muscle exposed.
Advantages include a low risk of tonsillar regrowth and recurrence of symptoms. Disadvantages include higher postoperative pain and a longer recovery period.
PITA involves partial removal of the tonsils while preserving the tonsillar capsule. Surgeons use powered devices such as coblation or a microdebrider to remove most of the lymphoid tissue but leave a thin layer intact.
The rationale is that preserving the capsule reduces exposure of nerve endings and muscle, resulting in less pain, reduced bleeding, and faster healing.
However, leaving residual lymphatic tissue may also have biological consequences, including inflammation and immune activation.
Postoperative fever in children is common after many surgical procedures and is often benign. However, fever can cause significant anxiety for parents and may lead to unnecessary medical visits, antibiotic use, or hospital readmission.
Clinically, fever may be caused by:
Understanding whether surgical technique influences fever risk is essential for appropriate counseling and postoperative care.
The study was a prospective cohort study conducted at a tertiary referral center between June 1, 2023, and November 30, 2024.
A total of 82 children underwent tonsillectomy with or without adenoidectomy.
The primary outcome was postoperative fever defined as temperature greater than 37.9°C or 100.2°F within one week following surgery.
The overall one week postoperative fever rate was 24.4 percent.
Children who underwent PITA had significantly higher rates of fever compared to those who underwent cold adenotonsillectomy.
This means children in the PITA group were nearly five times more likely to experience fever during the first postoperative week.
Parents of children who underwent PITA were more likely to seek medical evaluation postoperatively.
This difference was statistically significant and likely reflects parental concern related to fever rather than serious complications.
Despite higher fever rates, PITA showed clear advantages in recovery outcomes.
These findings are consistent with previous studies highlighting reduced morbidity with intracapsular techniques.
Importantly, there were no significant differences between groups in:
Most fever episodes were mild, self-limited, and managed conservatively at home.
The study authors suggest that postoperative fever after PITA may be related to inflammatory activity in retained lymphatic tissue.
Possible mechanisms include:
Unlike cold tonsillectomy, which removes the entire lymphoid structure, PITA leaves behind tissue capable of mounting an inflammatory response.
Importantly, this does not necessarily indicate infection.
Parents should understand that mild fever after tonsil surgery, especially following PITA, is often part of the normal healing process.
Most fevers in the study did not require antibiotics, hospitalization, or invasive evaluation.
Parents should seek medical advice if:
Clear postoperative instructions can significantly reduce anxiety and unnecessary clinic visits.
Surgeons should incorporate these findings into preoperative counseling.
Key points to discuss include:
Setting expectations may reduce unplanned healthcare utilization and improve satisfaction.
No tonsillectomy technique is without trade-offs.
| Outcome | Cold Adenotonsillectomy | PITA |
|---|---|---|
| Postoperative pain | Higher | Lower |
| Return to diet | Slower | Faster |
| Fever risk | Lower | Higher |
| Tissue regrowth | Minimal | Possible |
| Bleeding risk | Comparable | Comparable |
The choice of technique should be individualized based on patient age, indication for surgery, surgeon experience, and family preferences.
Powered intracapsular tonsillectomy and adenoidectomy continues to be an attractive option for pediatric patients due to reduced pain and faster recovery. However, evidence now shows that it is associated with higher rates of postoperative fever during the first week after surgery.
These fevers are typically mild, inflammatory in nature, and manageable with conservative care. Proper parental education and reassurance are essential to prevent unnecessary anxiety and medical visits.
As surgical techniques evolve, understanding not only the benefits but also the expected postoperative course is key to delivering high quality, family centered care.
Noy R, Barzilai R, Khoury EE, Gordin A. Intracapsular Tonsillectomy and Adenoidectomy Is Associated With Higher Rates of Postoperative Fever: A Prospective Cohort Study. Clinical Otolaryngology. First published December 30, 2025. DOI: 10.1111/coa.70078
This article is intended for educational and informational purposes only and does not constitute medical advice. It is not a substitute for professional diagnosis, treatment, or consultation with a qualified healthcare provider. Parents and caregivers should always seek the advice of their child’s physician or surgeon regarding postoperative symptoms or concerns.

Most Accurate Healthcare AI designed for everything from admin workflows to clinical decision support.